 This is Nadia’s story told by her mother, Tasha. Thank you for sharing Nadia with us!
This is Nadia’s story told by her mother, Tasha. Thank you for sharing Nadia with us!We found out at our 20 week anatomy scan that something was wrong with Nadia’s heart. By 24 weeks we had her full diagnosis: HLHS, DORV, TGA, and Pulmonary Atresia. All caused by heterotaxy syndrome which also caused her stomach, liver, and spleen to be on the wrong side of her body. Nadia was born October 15, 2013 at Vanderbilt hospital. She had her first surgery, the Norwood, at a week old. That night she also had her second open-heart surgery when the shunt that they placed during her Norwood clotted and she was rushed back to surgery to place a new one. She came home when she was 3 weeks old.
At three months old she had her third surgery the Glenn. The night of the surgery she had many complications causing the doctors to open her chest u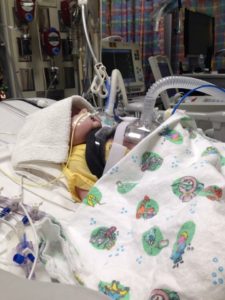 p and send her to have an emergency heart cath to remove a clot that was pressing on one of her vessels. By morning she was placed on ECMO (life support) and would stay on it for the next 5 days and her chest remained open for 10 days. This was by far the worst night of my life, not knowing if she would make it through the night or not. We were told by one of the nurses the next morning that Dr. Maynard did not leave her side all night. While on ECMO she had a stroke that affected her right side.
p and send her to have an emergency heart cath to remove a clot that was pressing on one of her vessels. By morning she was placed on ECMO (life support) and would stay on it for the next 5 days and her chest remained open for 10 days. This was by far the worst night of my life, not knowing if she would make it through the night or not. We were told by one of the nurses the next morning that Dr. Maynard did not leave her side all night. While on ECMO she had a stroke that affected her right side.
Over the next month she seemed to be improving and working towards going home. However she was unable to come completely off of oxygen. She was sent back for another heart cath that showed her body had formed over 50 collateral vessels to her right lung. The doctors gave us two options the first to leave everything how it was and bring her home knowing that her body would continue to damage the right lung which would mean that she would not be able to have the next needed surgery, the Fontan. The second option was to take her back to surgery and take down the Glenn that was going to her right lung and place a shunt. We chose the second option.
She had her fourth surgery in march. Surgery went well. A week after surgery her chest incision started to look red and inflamed, and later that day the entire incision opened up. They took cultures and placed a wound vac. The cultures came back positive for serratia. She was started on 6 weeks of antibiotics and was discharged  with a picc line and iv antibiotics.
with a picc line and iv antibiotics.
She was home for a week when we finished the antibiotics, two days later the infection was back and this time it came back as MRSA. She spent the next couple of weeks in the ICU because the infection also caused necrotizing enterocolitis (nec). She was put on another 6 weeks of antibiotics and the infection came back again after the antibiotics were stopped. This time she came home with a wound vac and 12 weeks of antibiotics. She was discharged in June and has been home since.
weeks in the ICU because the infection also caused necrotizing enterocolitis (nec). She was put on another 6 weeks of antibiotics and the infection came back again after the antibiotics were stopped. This time she came home with a wound vac and 12 weeks of antibiotics. She was discharged in June and has been home since.
She is doing well now, she still has severe oral aversions and does not eat by mouth but developmentally she is catching up to other kids her age and is just busy being a happy active girl while we wait to see what her next surgery step will be.