Every CHD story is different. Raleigh’s is unique because he was not diagnosed until he was nearly 9 months old. Looking back, there were signs early on, but hindsight is so often 20/20. Before he was born, we had several extra ultrasounds to watch 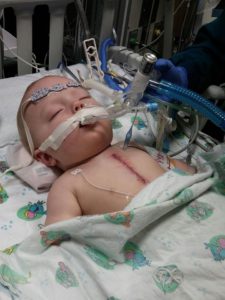 Raleigh’s kidneys which were always distended, but then at birth his kidney function was fine. Raleigh was born at 35 weeks, and although he was 5 weeks early he weighed 6 lbs and 2 oz and was 19 inches long. At four days old we were discharged from the hospital, and we went home as a family. We were encouraged to check in every day with our pediatrician for weight checks.
Raleigh’s kidneys which were always distended, but then at birth his kidney function was fine. Raleigh was born at 35 weeks, and although he was 5 weeks early he weighed 6 lbs and 2 oz and was 19 inches long. At four days old we were discharged from the hospital, and we went home as a family. We were encouraged to check in every day with our pediatrician for weight checks.
Raleigh had some issues feeding very early on, so his weight continued to drop. On day six, we rushed Raleigh to the emergency department at Monroe Carell Jr. Children’s Hospital at Vanderbilt. He was lethargic and unresponsive. His body temperature was less than 97 degrees, and he weighed a little more than 5 lbs. The medical team ran a battery of tests, but nothing came back positive. It was determined that because he was premature, Raleigh was just too small to maintain his body temperature on his own. He was admitted to the NICU so he could “fatten up.”
During Raleigh’s stay in the NICU the attending physician mentioned that he had heard a faint heart murmur. He said it was not uncommon for preemies to have such murmurs, and most of them eventually disappear. We were encouraged not to be concerned about it, and ensured that our pediatrician would follow-up if there were any other issues. After 5 days in the NICU, Raleigh was nearly back up to his birth weight, and he was once again discharged to head home.
When Raleigh was about 8 months old, we were concerned that he might have an ear infection. When we took him to the pediatrician to have his ears checked, our doctor said something we had not heard since we had been in the NICU. The faint heart murmur the doctor in the NICU had heard was now a very pronounced heart murmur. We left that day with a referral to the Pediatric Heart Institute at Vanderbilt.
During our appointment with the cardiologist later that month, Raleigh was diagnosed with two congenital heart defects – coarctation of the aorta and bicuspid aortic valve. It was explained to us that the coarctation of the aorta was the most worrisome and in the simplest terms this meant Raleigh had a narrowing of a major blood vessel. This condition almost always requires surgery to repair the defect. We were told at the time our cardiologist wanted to wait until Raleigh was 4 or 5 years old to do the surgery.
 After a handful of follow-up appointments, on Valentine’s Day the following year, the day Raleigh turned 14 months old, we were told it was best to go ahead and schedule the surgery. Raleigh’s pressures and gradients were rapidly worsening, and the repair needed to be made sooner rather than later. Raleigh’s surgery was scheduled for early April, and we were sent home with blood pressure meds.
After a handful of follow-up appointments, on Valentine’s Day the following year, the day Raleigh turned 14 months old, we were told it was best to go ahead and schedule the surgery. Raleigh’s pressures and gradients were rapidly worsening, and the repair needed to be made sooner rather than later. Raleigh’s surgery was scheduled for early April, and we were sent home with blood pressure meds.
The next couple of months were a whirlwind getting ready for Raleigh’s surgery. Raleigh presented as a bit of an enigma to the cardiology team. As his surgery date approached and more imaging tests were conducted, the team began to suspect that in addition to coarctation of the aorta, Raleigh also had aortic arch hypoplasia. This was a significant diagnosis because the original plan was to do the repair through a small incision between Raleigh’s ribs under his arm while his heart and lungs would continue to operate on their own. The additional diagnosis of the aortic arch hypoplasia meant that Raleigh’s entire arch would need to be rebuilt. He would require open heart surgery on bypass (meaning his heart would be stopped and a machine would perform his heart and lung functions during the surgery).
Raleigh’s heart team did an amazing job on his surgery and in facilitating his recovery. After a year and a half of various medications and very frequent doctor’s visits, Raleigh has graduated to annual cardiology check-ups and he is no longer taking  any daily medications for his heart. We are currently watching some scar tissue that resulted from his open heart surgery in hopes that it does not cause additional narrowing that would need to be addressed. He will follow-up with a cardiologist for the rest of his life, and most likely when he is around 40 years old, he will need to have his bicuspid valve replaced.
any daily medications for his heart. We are currently watching some scar tissue that resulted from his open heart surgery in hopes that it does not cause additional narrowing that would need to be addressed. He will follow-up with a cardiologist for the rest of his life, and most likely when he is around 40 years old, he will need to have his bicuspid valve replaced.
We are so blessed to have a healthy boy who can do pretty much whatever any other three-and-a-half year old can do. During the past three years we have been immersed in a community of other CHD families. This community has supported us through so much. Before Raleigh’s diagnosis, we didn’t know much about CHD, so we now spend a lot of our time trying to raise awareness and money for CHD research and patient support. We are thrilled about the work that Project Heart is doing to help CHD patients and their families!