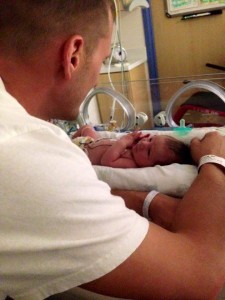
 Trace’s diagnosis came right on the edge of 24 weeks gestation. We had gone for the 20 week anatomy scan and the tech said she couldn’t get a good shot of his heart because he was really squirmy. We went back at 24 weeks and she scanned for nearly an hour. I knew we had gone over our allotted time and I was concerned. She, of course, couldn’t and wouldn’t answer any questions. She and the doctor stood together outside the room for several minutes before he came in. He repeated what he had said 4 weeks earlier. “We can’t see it, but that doesn’t mean anything is wrong. We want to send you to a maternal fetal specialist.” I held my composure thinking they were just needing better pictures. He’s the fourth child, three healthy ones before, surely my body knew what it was doing by now? My best friend came with me to the third scan since my husband, Kenneth, had worked the night before and was working again the next night. When the
Trace’s diagnosis came right on the edge of 24 weeks gestation. We had gone for the 20 week anatomy scan and the tech said she couldn’t get a good shot of his heart because he was really squirmy. We went back at 24 weeks and she scanned for nearly an hour. I knew we had gone over our allotted time and I was concerned. She, of course, couldn’t and wouldn’t answer any questions. She and the doctor stood together outside the room for several minutes before he came in. He repeated what he had said 4 weeks earlier. “We can’t see it, but that doesn’t mean anything is wrong. We want to send you to a maternal fetal specialist.” I held my composure thinking they were just needing better pictures. He’s the fourth child, three healthy ones before, surely my body knew what it was doing by now? My best friend came with me to the third scan since my husband, Kenneth, had worked the night before and was working again the next night. When the scan was finished, the doctor set down a box of Kleenex in front of me. He told me Trace had Tricuspid Atresia and possibly a completely closed off pulmonary artery. I asked if this was something that could be repaired he said, “This is above my pay grade. It happens a lot but it’s something only Vanderbilt can take care of in this area.” He told me that the problem is that he would have limited, if any, oxygen at birth.
scan was finished, the doctor set down a box of Kleenex in front of me. He told me Trace had Tricuspid Atresia and possibly a completely closed off pulmonary artery. I asked if this was something that could be repaired he said, “This is above my pay grade. It happens a lot but it’s something only Vanderbilt can take care of in this area.” He told me that the problem is that he would have limited, if any, oxygen at birth.
The ride home was exceptionally quiet. My friend did all she could to make me feel better. I got home and woke up Kenneth. I couldn’t even get it all out, I had to let him read the paper that the doctor had written and show him the picture he drew. I couldn’t say it. My oldest had a baseball game that afternoon and I had to get myself together before then. My appointment at Vanderbilt hadn’t been set and I had convinced myself that if Vanderbilt wasn’t in a hurry, I shouldn’t be too concerned. They called from the cardiology office while we were at the ball game that evening.. They shouldn’t have been in the office that late.. They set my appointment for 3 days from then. They were not only in a hurry, they were staying late. Dr. Parra confirmed the Tricuspid Atresia but said there was only a pulmonary stenosis and they could work around it. He described in detail what each step (BT shunt, Glenn &  Fontan surgeries) would do for Trace’s heart. He told us that “contact sports” would be out of the question. My mind flashed back to just days before watching my oldest slide into home and the catcher behind the plate. That was contact. They’re all contact sports. I was terrified and overwhelmed.
Fontan surgeries) would do for Trace’s heart. He told us that “contact sports” would be out of the question. My mind flashed back to just days before watching my oldest slide into home and the catcher behind the plate. That was contact. They’re all contact sports. I was terrified and overwhelmed.
Trace had his first open heart surgery at 7 days old. They placed a BT shunt and tied his PDA. That night all of our family had gone home and Kenneth was sleeping in the waiting room while we waited for the key to a sleep room outside the ICU. I walked into his room and he was blue. I woke Kenneth and he walked in just as they were giving Trace more medicine and said Dr. Mettler was on his way. Why in the world would the surgeon be coming back? Suddenly there were 10+ people in his room. We sat in the back of the room until Dr. Mettler came and told us what was happening. Trace’s shunt wasn’t working. His body wasn’t getting any oxygen. Cue my only real sobbing, can’t catch my breath break down. Dr. Mettler told us he had it all under control and asked Kenneth to take me to get a breath of fresh air. He re-opened his chest right there in the room, untied his PDA so he could get oxygen again, left his chest open for the night, and the next morning he reassembled his team. They took out the BT shunt and changed it to a larger central shunt and retired his PDA. This new shunt held him over until he was 4 months old and he went back for his third heart surgery, the Glenn.
Cue my only real sobbing, can’t catch my breath break down. Dr. Mettler told us he had it all under control and asked Kenneth to take me to get a breath of fresh air. He re-opened his chest right there in the room, untied his PDA so he could get oxygen again, left his chest open for the night, and the next morning he reassembled his team. They took out the BT shunt and changed it to a larger central shunt and retired his PDA. This new shunt held him over until he was 4 months old and he went back for his third heart surgery, the Glenn.
We are hoping that does the trick for as long as possible but we’ve been told to expect his next surgery around 2 and a half to 3 years old. Like all with a single ventricle Fontan repair, we hope it lasts forever, but it is likely he may need a revision surgery in his late teens to early twenties.
Now Trace is a happy, fun-loving 19 month old. He loves his brother and sisters and squeals everyday when they come through the door. He is the funniest person he knows. He will do anything he thinks will make you (or him) laugh. And he has no apparent interest in ever saying the word “momma” 🙂